 Have you ever had an eye infection? A case of dry eye? Horrible allergies? If you are like most people, at some point in your life, you have had to use those pesky eye drops. Eye drops can be irritating, difficult to use, and at times it seems as if more of the solution drips down your face than makes it in your eye. They are an imperfect solution to a myriad of vision problems. However, clinicians and scientists at the University of Pittsburgh are working to improve eye drop technology and revolutionize the way we deliver medicine to the eye.
Have you ever had an eye infection? A case of dry eye? Horrible allergies? If you are like most people, at some point in your life, you have had to use those pesky eye drops. Eye drops can be irritating, difficult to use, and at times it seems as if more of the solution drips down your face than makes it in your eye. They are an imperfect solution to a myriad of vision problems. However, clinicians and scientists at the University of Pittsburgh are working to improve eye drop technology and revolutionize the way we deliver medicine to the eye.
Current Eye Drop Needs and Drawbacks
There are approximately 3 million people with glaucoma and between 16 and 49 million people suffering from dry eyes in the United States alone. Add in patients suffering from infections or inflammatory diseases (uveitis), and that is a significant number of people who have to administer eye drops regularly. Some barriers to using eye drops include poor eyesight, coordination issues, and musculoskeletal disease (arthritis). Additionally, adherence to treatment with eye drops is poor, with patients having trouble with the frequency of dosing, correct usage, and wastage of drops.
A solution to many of these issues is a sustained release drug delivery system that lowers the dosage frequency. “I think we’re all fairly familiar with sustained or extended-release drugs when it comes to other medications, such as taking a pill once a day,” says Ian Conner, MD, PhD, an Assistant Professor of Ophthalmology, Glaucoma and Cataract Service. “This principle can apply to eye drops as well, and instead of frequent eye drops, we can hopefully bring it down to monthly dosing, or even less frequent than that.”
The Future of Ocular Drug Delivery
While there are currently several options for this type of medication on the market, such as Ocusert, Dextenza, Ozurdex, and Durysta, these treatment options carry with them their own drawbacks such as discomfort in the eye, inconsistent biodegradability, collateral damage to adjacent tissue, and the reversal/removal can be invasive. Scientists within the department are developing a new drug delivery system that will be long-lasting and non-invasive, making dosage easier and convenient for patients with glaucoma, dry eye, and other diseases.
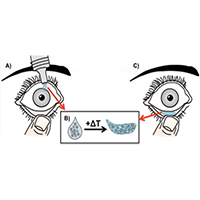
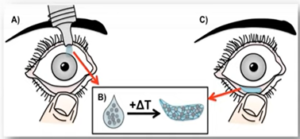
Morgan Fedorchak, PhD, and her team are currently developing a product they call SoliDrop, a long-term gel eye drop that would be self-administered monthly. “Even though the technology within the SoliDrop eye drop is very advanced, the act of administering an eye drop is very familiar to these patients.” The product itself is quite remarkable, as the eye drop is a liquid at room temperature. However, when heat is applied, it takes on a solid, gel-like state. This means that as the eye drop enters the eye, it is heated into a very flexible and comfortable gel that sits in the lower eyelid and conforms to the size and space of the eye. “One of the things that we were very concerned about was removal,” says Dr. Fedorchak, an Assistant Professor of Ophthalmology, Bioengineering, and Clinical & Translational Sciences. “All a patient has to do is flush their eye with water, and the gel will slide right out, making removal quick and simple for patients handle themselves.”
Additional advantages of this delivery system include:
- Less drug = fewer side effects (same therapeutic effect)
- No need for preservatives (can be stored at room temperature)
- Won’t block vision or interfere with contact lenses
- Easy to see and remove
While not available for clinical trials yet, early testing results show that this drug can treat glaucoma patients for up to 28 days, help prevent infection, simultaneously deliver two different drugs, and can cut the treatment schedule for cystinosis from hourly eye drops to daily, which would be an incredible ease of burden on patients suffering from this disease.
This innovative research is only made possible with support from generous donors to the Eye & Ear Foundation. If you would like to be a part of this groundbreaking work being done, please consider making a gift to help support our research.